Missing teeth are more than a cosmetic concern — they affect how you chew, speak, and how the jaw ages over time. Dental implants have become the go-to solution for replacing one or many teeth because they restore function as well as appearance. Implants recreate the tooth root and support a wide range of restorations, helping patients regain confidence and normal oral function.
Advances in materials and digital planning have made implant therapy predictable and adaptable to many different situations. From single-tooth replacements to full-arch restorations, implants give clinicians the ability to design outcomes that look natural and perform reliably for years. This predictability is a major reason implants are now considered a standard of care for long-term tooth replacement.
At Diamond Head Dental Care in Pearl City, our approach blends modern techniques with personalized treatment planning. We emphasize clear communication and careful evaluation so that each implant plan fits the patient’s oral health, lifestyle, and esthetic goals.

A dental implant is a small, biocompatible post — typically titanium or a titanium alloy — surgically placed into the jawbone. Over time the bone fuses to the implant in a process called osseointegration, creating a stable foundation that behaves much like a natural tooth root. Once integrated, the implant can support crowns, bridges, or denture systems that feel secure and function naturally.
Because the implant supports the prosthetic from within the bone, the result preserves chewing efficiency and speech patterns better than removable options. Patients often note that foods taste the same and speaking feels unaffected, thanks to the stability implants provide. The prosthetic tooth is tailored in shape, color, and position to match surrounding teeth for a seamless appearance.
Long-term success depends on thoughtful planning and ongoing oral hygiene. With precise placement and routine maintenance, implants offer durable, comfortable support for replacement teeth without relying on neighboring natural teeth for stability.
Successful implant therapy begins with a comprehensive evaluation that looks at bone volume, gum health, bite relationships, and overall medical history. Modern diagnostics, including digital X-rays and 3D imaging, allow clinicians to visualize anatomy and plan implant positions to avoid critical structures and maximize support.
The timeline for implant treatment varies. Some patients receive a temporary restoration immediately after surgery, while others follow a staged approach where the implant integrates before the final prosthetic is attached. Your clinician will explain the recommended sequence based on clinical findings and desired outcomes.
Communication about anesthesia and comfort options is part of preoperative planning. We provide clear instructions and reassurance so patients know what to expect before, during, and after implant placement.
Implants deliver a combination of functional and biologic advantages that set them apart from traditional tooth replacement options. Because they anchor restorations directly to the jawbone, implants maintain chewing strength and reduce the risk of movement or slippage that can occur with removable dentures.
Another key benefit is preservation of the jawbone. When a tooth is lost, the underlying bone can slowly resorb without stimulation. Implants recreate that stimulation and help preserve natural facial contours, supporting a more youthful profile over time.
Additional practical benefits include long-term stability, minimal impact on neighboring teeth, and restorations that rarely require extensive adjustment once properly placed. With good hygiene and regular professional care, implant-supported teeth can remain an effective solution for many years.
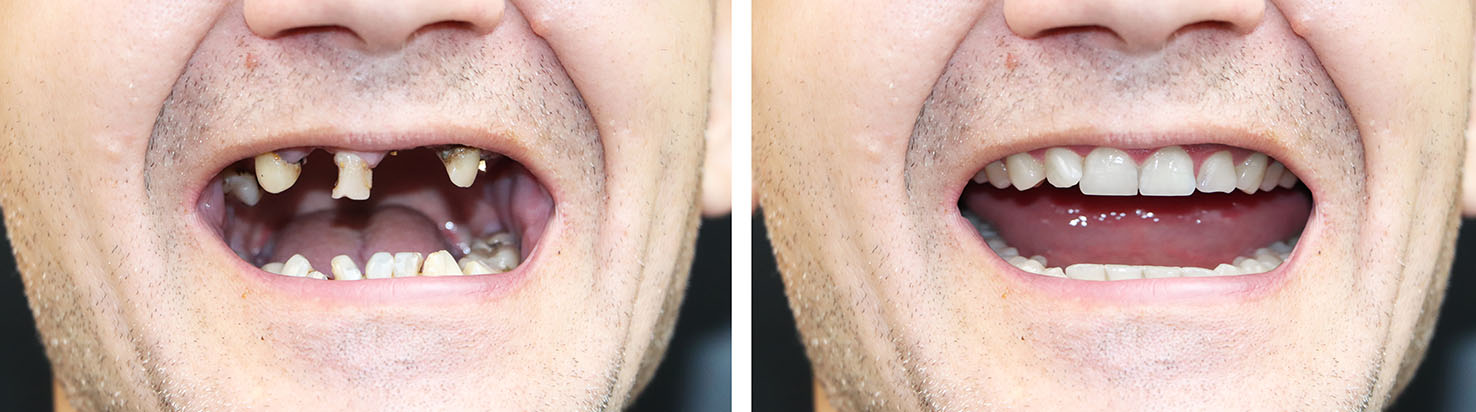
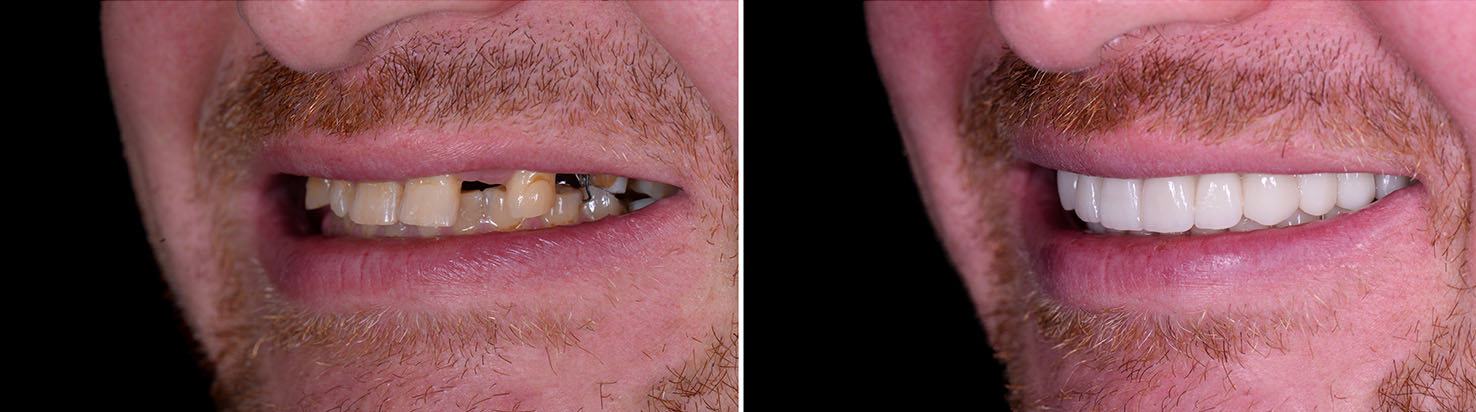
A single implant restored with a custom crown replaces one missing tooth without touching neighboring teeth. This approach conserves the structure of adjacent teeth because it eliminates the need for a traditional bridge, which typically requires altering nearby healthy teeth for support.
Single-tooth implants are predictable and esthetic, making them a preferred option for visible areas of the smile. The crown is crafted to match the size, shape, and color of natural teeth so the result blends in seamlessly.
For suitable candidates, a single implant often represents the most conservative long-term choice for replacing an isolated missing tooth.
When two or more adjacent teeth are missing, an implant-supported bridge can replace them without relying on natural teeth as anchors. Strategically placed implants act as supports for a multi-unit restoration, maintaining bone stimulation and preserving the health of remaining teeth.
This option minimizes the sacrifice of healthy dental structure and provides a durable, fixed restoration with strong chewing capability. Implant-supported bridges are a valuable alternative to removable partial dentures.
The number and placement of implants depend on the span of missing teeth, bone anatomy, and the desired cosmetic outcome.
For patients missing an entire arch of teeth, implant-supported full-arch replacements restore function and esthetics in a way that conventional dentures cannot. Depending on the plan, a set of four to six implants can support a fixed bridge or a secure overdenture, both of which improve stability and chewing efficiency.
Some protocols allow for immediate placement of temporary teeth on the same day as implant surgery, offering a quick restoration of appearance and function while the implants integrate. The final prosthesis is delivered once healing is complete for optimal fit and longevity.
Full-arch implant solutions eliminate many of the limitations associated with traditional dentures and significantly enhance quality of life for appropriate candidates.
Implant-retained dentures attach to a few carefully placed implants and offer enhanced retention compared with conventional removable dentures. These hybrid solutions provide a secure fit while still allowing the prosthesis to be removed for cleaning, offering a practical balance for many patients.
By reducing movement and improving bite stability, implant-retained dentures make eating and speaking easier and more comfortable. They are often recommended for patients who want improved denture function without a fully fixed restoration.
Determining candidacy begins with a full dental and medical assessment. We review gum health, the condition of adjacent teeth, bite relationships, and systemic factors that could affect healing. Digital imaging helps us assess bone volume and identify the ideal implant sites.
Patients with controlled systemic conditions and adequate bone are commonly suitable candidates. When bone is insufficient, preparatory techniques like bone grafting or sinus augmentation can create a stable foundation for implants.
We tailor treatment based on each patient’s needs and goals, taking time to explain options and expected timelines so you can choose the approach that fits your life.
Implant therapy is a multi-step process that begins with diagnostic planning and may include preparatory treatments such as extractions or bone grafts. The implant is then placed in the jawbone during a minor surgical procedure performed under controlled conditions.
After placement, a healing period allows the implant to integrate with the bone. During this time, a temporary restoration can often be used so daily life is minimally affected. Once osseointegration is complete, a custom abutment and final prosthesis are fabricated and attached to achieve the desired form and function.
Follow-up care includes routine check-ups and professional cleanings to monitor the implant and surrounding tissues. With proper maintenance, implant-supported restorations are an enduring solution for many patients.
Bone loss is common after tooth loss or chronic gum disease, and adequate bone volume is essential for long-term implant stability. When imaging shows insufficient bone, grafting procedures add volume and create a secure base for implant placement. These grafts can use bone from the patient, donor material, or synthetic substitutes depending on the clinical situation.
Bone grafting is a routine part of many implant treatment plans and is performed to optimize the position, support, and longevity of the implant restoration.
Dental implants offer realistic, long-lasting results for many patients, combining function, health benefits, and esthetic improvements. Choosing a provider who emphasizes careful planning, modern diagnostics, and individualized care is essential to a successful outcome.
At Diamond Head Dental Care, our team focuses on clear communication and evidence-based approaches to help patients explore implant options that meet their needs. We strive to make the process understandable and predictable so you can make confident decisions about your oral health.
If you’re considering implants or want to learn whether they’re the right solution for your smile, contact us to discuss your options and schedule a consultation. We’ll review your unique situation and outline a thoughtful plan to help you rebuild a healthy, functional smile.
If you've lost a tooth due to injury, decay, gum disease, or any other reason, we recommend dental implants to replace missing teeth. Dental implants come the closest to replicating the look, feel, and function of your natural teeth.
Dental implants are placed into the jawbone and mirror the same function as the root of a tooth. The procedure for dental implants is usually performed while a patient is sedated. Patients who undergo IV sedation must have an empty stomach and transportation home following the procedure. Most sedation patients will have little to no memory of the procedure occurring.
Generally, dental implants are made out of a biocompatible metal such as titanium. Biocompatible metals are also used for other common bone implants (such as shoulder, hip, and knee replacements). The visible portion of the implant is usually made out of porcelain and is custom-made to match your existing teeth.
Dental implants are designed to fuse to the bone, which makes them become permanent fixtures. Typically speaking, the success rate is nearly 100%. There are few cases in which the implant will not fuse as intended and must be removed. If this happens to occur, the procedure can be attempted again a few months later.
Dental implants are not usually covered by dental insurance, but may be covered under a patient's medical insurance. Our office and your insurance company can discuss coverage options with you based on your individual case and treatment plan.
It's easy... just take care of an implant as if it's a natural tooth! This involves regular brushing, flossing, and dental checkups. If you have any concerns about your implant, contact us immediately.
Dental implants are small, biocompatible posts, most often titanium or a titanium alloy, that are placed into the jawbone to replace missing tooth roots. Over weeks to months the surrounding bone fuses to the implant in a process called osseointegration, creating a stable foundation for a prosthetic tooth. Once integrated, the implant supports a crown, bridge, or denture that restores chewing, speech and appearance in a way that closely mimics a natural tooth.
The prosthetic tooth is custom fabricated to match adjacent teeth in size, shape and color so the result looks seamless. Because the implant is anchored in bone, it preserves chewing efficiency and reduces movement or slipping that can occur with removable options. Long-term success depends on careful planning, precise placement and consistent oral hygiene to keep the surrounding tissues healthy.
Good candidates typically have healthy gums, sufficient jawbone volume or a willingness to undergo preparatory grafting, and overall health that supports surgical healing. Many systemic conditions can be managed so patients still qualify, but a complete medical and dental history helps clinicians identify factors that may affect outcomes. Habits such as tobacco use and uncontrolled conditions like diabetes can increase risk and are assessed during planning.
Candidacy is determined through a comprehensive evaluation that includes clinical examination and modern imaging such as digital X-rays or 3D CBCT scans. These diagnostics reveal bone anatomy and critical structures so the treatment team can recommend appropriate implant types or preparatory procedures. When bone is insufficient, bone grafting or sinus augmentation can often create a reliable foundation for implants.
Implant therapy typically begins with a consultation and diagnostic imaging, followed by any necessary preparatory care such as extractions or bone grafting. The implant is placed during a minor surgical procedure performed under local anesthesia and, if desired, sedation options; after placement the implant requires a healing period for osseointegration. During healing many patients receive a temporary restoration so daily function and appearance are maintained.
Once integration is confirmed, a custom abutment and final prosthesis are fabricated and attached to achieve proper fit, function and esthetics. The total timeline varies by clinical complexity, ranging from a few months for staged approaches to shorter timelines when immediate protocols are appropriate. Routine follow-up visits and professional cleanings are scheduled to monitor the implant and surrounding tissues for long-term health.
Implant restorations are tailored to the number and location of missing teeth and can include single crowns, implant-supported bridges, implant-retained dentures, and full-arch fixed bridges. Single crowns replace one tooth without altering adjacent teeth, while implant-supported bridges replace multiple adjacent teeth using implants as anchors. Implant-retained overdentures attach to a small number of implants for improved retention and ease of care, and full-arch solutions can restore an entire upper or lower jaw with a fixed or removable prosthesis.
The choice of restoration depends on bone anatomy, esthetic goals and functional needs, and some protocols allow for provisional teeth on the day of surgery to expedite restoration of appearance and chewing. Advanced planning and digital workflows improve predictability for each restoration type. Your clinician will recommend the option that best balances durability, hygiene access and the long-term health of surrounding tissues.
Bone grafting restores deficient jawbone volume so an implant can be placed in an optimal position for long-term stability and esthetics. Grafts may use the patient’s own bone, donor material, or synthetic substitutes depending on the clinical need and the size of the defect. Common grafting approaches include ridge augmentation to rebuild a narrow jaw and sinus lifts to increase height in the upper jaw when the sinus floor is close to the planned implant site.
After grafting, a healing period allows the graft to integrate and consolidate with native bone before implant placement or in some cases before final restoration. The timeline and technique are selected based on your anatomy and treatment goals, and careful imaging guides the process to reduce complications. When properly planned and executed, grafting dramatically increases the pool of patients eligible for implant therapy.
Daily care for implant-supported teeth follows the same fundamentals as natural teeth: brush twice a day with a soft-bristled brush and use interdental cleaning such as floss, interdental brushes or water flossers to remove plaque around abutments and prosthetic margins. Pay special attention to the junction between the implant restoration and gum tissue, where plaque can lead to inflammation if neglected. Avoid tobacco and adopt healthy habits that support healing and gum health.
Professional maintenance is also essential; schedule regular dental exams and cleanings so your clinician can monitor peri-implant tissues and address early signs of inflammation. The frequency of visits may be individualized based on your risk profile and the type of restoration. Prompt attention to any redness, swelling or increased mobility helps protect the long-term success of the implant.
Dental implants are generally predictable, but like any surgical treatment they carry potential risks such as infection, failure of osseointegration, nerve irritation, sinus complications, or peri-implant inflammation. Careful diagnostics, precise surgical technique and good patient health reduce the likelihood of these events. Early detection through routine follow-up is important because many complications are easier to treat when identified promptly.
Management depends on the specific issue and may include antibiotics for infection, nonsurgical therapy and improved hygiene for peri-implant mucositis, or surgical intervention for persistent problems. In rare cases a failed implant can be removed and the site rehabilitated with additional grafting before replacement. Open communication with your clinician about symptoms and risk factors helps guide effective, conservative solutions.
Local anesthesia is the standard for implant placement and provides reliable pain control during the procedure, while sedation options such as nitrous oxide, oral sedatives or IV sedation are available for patients with anxiety or complex surgical needs. Your clinician will review medical history and preferences to recommend an approach that maximizes comfort and safety. Preoperative instructions and clear communication about what to expect help reduce stress on the day of surgery.
Aftercare commonly includes short-term prescription or over-the-counter analgesics, cold compresses to limit swelling, and written guidelines for diet and activity during healing. Following postoperative instructions closely reduces discomfort and supports successful integration. If concerns arise during recovery, prompt contact with the dental team ensures timely assessment and care.
Implants help preserve jawbone by transmitting normal chewing forces to the bone, which maintains stimulation and slows the resorption that typically follows tooth loss. By preserving bone height and volume, implants support the soft tissues and facial contours that contribute to a natural, youthful appearance. This structural benefit contrasts with removable dentures, which may accelerate bone loss where no root stimulation exists.
Maintaining peri-implant tissue health through hygiene and professional care is essential to preserve these benefits long term. Adequate bone support and proper restoration design also reduce the risk of mechanical complications and improve the predictability of outcomes. When planned with an eye toward both function and esthetics, implants can be a durable foundation for maintaining oral and facial health.
Your first implant consultation includes a thorough review of your medical and dental history, a clinical exam and diagnostic imaging to evaluate bone volume and anatomic relationships. The clinician will discuss your goals and explain the treatment options that fit your anatomy, including whether preparatory procedures like extractions or grafting are needed. You will receive a clear explanation of the anticipated sequence of care, typical timelines and the follow-up required to monitor healing.
At Diamond Head Dental Care in Pearl City we take time to answer questions and tailor a plan that balances functional needs and esthetic preferences for each patient. Expect a collaborative discussion that covers anesthesia choices, maintenance requirements and what to expect during recovery so you can make an informed decision about implant therapy. If further referrals or advanced imaging are recommended, the team will coordinate next steps to keep the process efficient and well organized.
